People Who Stay Energetic at 80 All Share This One Secret—And It’s Not What You Think
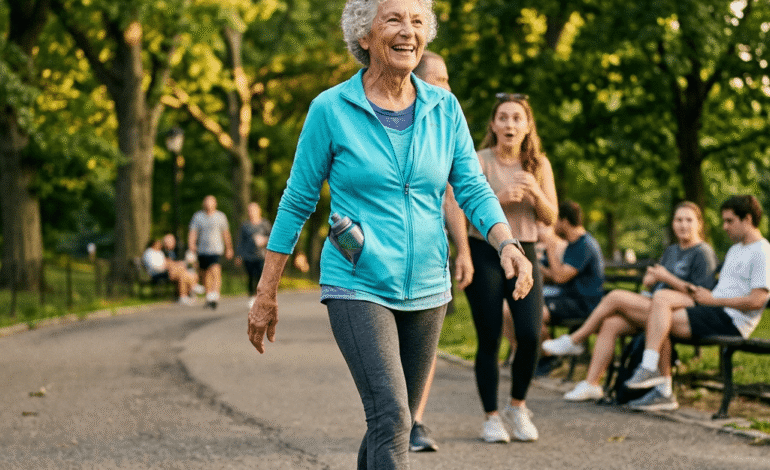
The Secret to Still Being Fully Alive at 80 (It Has Nothing to Do With Luck)
There’s a man in his mid-eighties who walks into his local library every Tuesday morning. He doesn’t go to pick up books — though he does that too. He goes because Maria, the librarian, always has the crossword pulled up on the desk, and the two of them argue over five-letter words for at least twenty minutes before he settles into his chair by the window.
He had a triple bypass at seventy-two. His wife of forty-one years passed away when he was seventy-eight. His knees have been unreliable since his late sixties.
And yet, if you watched him walk through those library doors, you would never describe him as someone fading. You would describe him as someone who still has somewhere to be.
Now picture someone else — a woman who retired at sixty-five into what looked, on the surface, like the reward of a life well-lived. A comfortable home. A loving family nearby. Enough savings to stop worrying. By seventy-nine, she was spending most of her days in front of the television, not quite sick, not quite well, slowly losing the threads of herself.
Both of these people made it to the same decade. What separated them had almost nothing to do with genetics, income, or even physical health. It had everything to do with something far less visible, and far more powerful.
The Decade That Science Has Finally Started Taking Seriously
For most of medical history, turning eighty was treated as a kind of finish line crossed against the odds. The conversation about health in older age focused almost entirely on managing decline — which diseases to watch for, which functions would slow, which losses to expect and accept.
That conversation is changing.
Researchers who specialize in gerontology — the science of aging — have spent the last decade trying to understand not just why people decline, but why some people don’t. Why certain eighty-year-olds remain sharp, engaged, and socially rooted while others disengage far sooner than their physical health would seem to require.
What they found is both simpler and more nuanced than most people expect. The trajectory of your eighties is being shaped right now, by choices that seem small and ordinary but compound over time into something profound. And the science behind it points to four interlocking forces that, when working together, create what researchers have begun calling an “upward spiral” — a self-reinforcing cycle of vitality that is available to almost everyone, at almost any age.
The forces aren’t exotic. They don’t require expensive supplements or extreme discipline. But they do require understanding what’s actually happening inside an aging body and mind — because that understanding changes everything.
The First Force: Purpose Isn’t Soft. It’s Survival.
Let’s start with the one that gets dismissed most often as being “nice to have.”
Purpose.
The word can sound abstract, almost motivational-poster-ish. But researchers studying populations with unusually high concentrations of centenarians have found something striking: the people who live longest, and live best, aren’t necessarily the ones with the best cholesterol numbers or the cleanest diets. They are, almost universally, the ones who have a reason to get out of bed that feels meaningful to them.
In Okinawa, Japan — one of the world’s famous “Blue Zones,” regions where people routinely live past one hundred — there isn’t even a word in the local dialect for retirement. The concept of removing yourself from meaningful participation in life simply doesn’t map onto how Okinawans think about growing older. What they have instead is the concept of ikigai — a Japanese term that translates roughly to “reason for being,” but means something more specific than that. It’s the intersection of what you love, what you’re good at, what the world needs, and what sustains you. For many elderly Okinawans, ikigai is not a grand mission. It’s tending a small garden. It’s making rice for a grandchild. It’s being the person on the block who notices when a neighbor’s light hasn’t come on in the morning.
The science behind why this matters is no longer speculative. A 2025 study published in The American Journal of Geriatric Psychiatry followed more than 13,000 participants and found that individuals who reported a stronger sense of purpose showed significantly less cognitive deterioration over time — even among people who carried genetic risk factors for conditions like Alzheimer’s. The purpose wasn’t just making their lives feel better. It was physically protecting their brains.
The mechanism appears to involve stress hormones. Chronic low-grade stress — the kind that comes from feeling redundant, invisible, or untethered from meaningful activity — keeps the body’s cortisol system in a state of low-level activation. Over months and years, this systemic stress accelerates inflammation, which damages both cardiovascular and neurological tissue. Purpose acts as a buffer against that kind of quiet physiological erosion.
Here’s the part that surprises people: the size of the purpose doesn’t seem to matter as much as the consistency of it.
Looking after a pet. Volunteering for two hours a week. Tending a plot in a community garden. Being the person in your family who calls to check in on everyone else. These are not small consolations. They are genuinely meaningful anchors, and the biology doesn’t distinguish between grand life missions and daily rituals of care. What matters is that something — or someone — is counting on your presence.
Curiosity matters too. Learning doesn’t have to stop at any age, and the brain responds to novelty with measurable neurological activity — new connections forming, old pathways being reinforced. An eighty-year-old who decides to learn how to use video calling software to see her grandchildren is doing something neurologically significant, even if it feels mundane. Every new skill, every answered question, every moment of figuring something out is a small act of resistance against the kind of withdrawal that accelerates cognitive decline.
The Second Force: Loneliness Is Not an Emotion. It’s a Health Crisis.
There’s a statistic that researchers cite so often it has almost lost its power to shock: chronic loneliness poses roughly the same risk to long-term health as smoking fifteen cigarettes a day.
Read that again, slowly. Fifteen cigarettes. Every day.
Most people, when they hear this, assume it must be a metaphor — a way of making an emotional truth sound more urgent. It isn’t. The mechanism is physiological. When humans — who are, at the deepest biological level, social animals — are cut off from meaningful connection over extended periods of time, the body interprets this as a danger signal. It activates the same stress-response systems that would switch on in the face of a physical threat. Cortisol rises. Inflammatory markers increase. The immune system shifts into a defensive posture that, maintained chronically, begins to damage the tissues it was meant to protect.
The heart suffers. The brain suffers. The research is consistent across dozens of studies and multiple countries: isolated older adults have dramatically higher rates of dementia, cardiovascular disease, and premature death than their socially connected counterparts.
And here’s the thing about reaching your eighties: the social world naturally shrinks. Friends pass away. Others move closer to their adult children. Mobility limitations make certain social activities harder. The workplace, which provided daily human contact for decades, is gone. The school-run conversations, the neighborhood routines — so much of what sustained social connection turns out to have been structural, built into the architecture of a working, active life. Remove the structure, and connection doesn’t automatically fill the vacuum.
The Harvard Study of Adult Development — one of the longest longitudinal studies of human wellbeing ever conducted, following participants across eight decades — found something that its researchers called “the most important finding” of the entire project. The quality of a person’s relationships at age fifty was a more reliable predictor of their physical health at eighty than their cholesterol levels.
Not their wealth. Not their fitness. Not even their mental health history. Their relationships.
What’s particularly hopeful about this finding is that connection doesn’t require large networks or intense friendships. Researchers studying social behavior in older adults have found that what they call “weak ties” — brief, warm interactions with the barista who remembers your order, the neighbor you wave to each morning, the librarian who argues with you about crossword answers — contribute meaningfully to wellbeing. The human nervous system responds to being seen and acknowledged, even in small doses.
The practical implication is this: in your eighties, social fitness is as important as physical fitness, and it requires the same intentional maintenance. A standing coffee date. A weekly card game. A phone call to a sibling every Sunday. These are not luxuries or indulgences. They are health interventions wearing ordinary clothes.
The Third Force: Your Body Is Still Listening to You
Here is where the conversation about aging most urgently needs updating.
The story most people carry into their later decades is a story of inevitable physical decline — a gradual but unstoppable reduction in capacity that accelerates with each passing year after a certain point. Rest more. Do less. Protect yourself from exertion. The body is fragile now.
The science tells a different story.
A landmark study published in 2026 in the Proceedings of the National Academy of Sciences found that exercise — even at modest intensity — triggers mitochondrial remodeling at the cellular level. Mitochondria are the energy-producing structures inside your cells, and their function naturally declines with age. But the study showed that physical activity sends a signal that causes cells to produce new mitochondria and repair damaged ones. In other words, movement doesn’t just make older bodies feel better. It reverses specific cellular processes associated with aging.
The goal of movement at eighty isn’t performance. It’s function.
Can you stand up from a chair without using your hands? Can you carry your own bags? Can you walk on uneven ground without losing your balance? These are the metrics that matter — not miles run or weights lifted. Geriatricians often use the “sit-to-stand” test as one of their primary assessments: can a person rise from a seated position, without pushing off with their hands, ten times in a row? The ability to do so correlates strongly with longevity and independence.
Muscle mass is the other urgent conversation. After the age of sixty, the body begins losing muscle tissue more rapidly than it can replace it — a process called sarcopenia. Left unaddressed, this loss of muscle is one of the primary reasons older adults become fragile, fall more easily, and lose independence. But it is not inevitable. Resistance training — using resistance bands, light dumbbells, or even body weight — directly counters sarcopenia by stimulating muscle protein synthesis. The muscles are not past listening. They respond to challenge at eighty just as they did at fifty. The stimulus just has to be there.
Walking, for its part, is more remarkable than it gets credit for. The impact forces generated by walking help maintain bone density, reducing fracture risk. Walking improves circulation, which benefits both the brain and the heart. And because it requires navigating the real world — its terrain, its people, its unpredictability — walking is also a cognitive activity. It keeps the body and mind working in tandem.
The Fourth Force: What You Feed an Aging Body Matters More, Not Less
One of the most persistent and damaging myths about eating in older age is that it becomes simpler — that the body needs less, demands less, tolerates less, and so the dietary calculus becomes easier.
In reality, the nutritional requirements of an aging body are more specific, not less.
The metabolism does slow. That part is true. But the demand for certain critical nutrients doesn’t slow with it. Protein, in particular, becomes more important as the body grows older, not less — because aging reduces the efficiency with which muscle tissue processes and uses dietary protein. To maintain muscle mass and prevent sarcopenia, older adults need more protein per kilogram of body weight than younger adults do, not less. The current evidence-based recommendation sits between 1.0 and 1.2 grams per kilogram of body weight per day.
And yet the most common dietary pattern among people in their eighties is what researchers drily describe as the “tea and toast” pattern — a diet of predominantly simple carbohydrates, chosen for convenience and ease of preparation. It’s not laziness. It’s a combination of factors: reduced appetite, difficulty cooking for one, dental changes that make certain foods harder to eat, and a food culture that doesn’t adequately support older adults in getting what they need.
Then there is the thirst gap — one of the stranger and less-discussed physiological changes that comes with age. The brain’s thirst-signaling mechanism becomes less reliable over time. Older adults experience the sensation of thirst far less acutely than younger people do, even when they are significantly dehydrated. The consequences of this are easy to miss and alarmingly serious: dehydration in older adults manifests as confusion, dizziness, falls, and urinary infections that can, in turn, cause sudden and dramatic changes in cognitive function. Hospital admissions for what looks like acute dementia sometimes turn out to be severe dehydration.
The solution isn’t complicated. It just requires making hydration a scheduled habit rather than a reactive one — drinking a glass of water with every meal and between meals, regardless of whether thirst signals the need. And ensuring that every meal contains a meaningful source of protein: an egg, some Greek yogurt, a portion of legumes, a piece of fish. Not complicated cuisine. Just intentional fuel.
How the Four Forces Become One: The Architecture of a Good Decade
The reason these four forces are so powerful isn’t just that each one matters individually. It’s that they feed each other.
Purpose gets you out of the house. Getting out of the house means moving your body. Moving your body brings you into contact with other people. Contact with other people elevates your mood and sharpens your mind. A sharper, more elevated mind makes you more likely to eat well, sleep better, and wake up the next morning with a reason to try again.
This is what researchers mean by the upward spiral. It’s not a motivational concept. It’s a description of a real biological and behavioral feedback loop — one that, once initiated, tends to be self-sustaining.
The inverse is equally true and equally important to understand. The downward spiral begins when one of these forces weakens. Isolation can kill purpose. The loss of purpose can kill motivation to move. Sedentary days can lead to poor nutrition. Poor nutrition can cloud cognition. Clouded cognition can make social connection feel overwhelming.
The practical wisdom here is that you don’t need to fix everything at once. You need to find the fallen domino and stand it back up. If energy is low, look at movement. If motivation is gone, look at connection. If mornings feel pointless, look for something small — something tiny and specific — that needs you to show up.
The Courage Nobody Talks About
There’s a kind of bravery that doesn’t get celebrated much, because it doesn’t look dramatic from the outside.
It’s the courage of an eighty-three-year-old who joins the Tuesday walking group at the community center even though she doesn’t know anyone there. It’s the courage of a man who signs up for a watercolor class he’s never tried, knowing he’ll be slow and clumsy at first. It’s the courage of reaching out to an old friend after years of silence, or of telling a doctor honestly how isolated you’ve been feeling, or of asking a grandchild to show you — again, patiently — how the video call works.
This is the courage that actually shapes a life in its final decades. Not the courage of dramatic moments, but the courage of daily showing up — of choosing visibility over withdrawal, curiosity over resignation, connection over the easier path of simply staying home.
The science is clear: the people who thrive past eighty are not the lucky ones. They are the ones who kept making small, consistent decisions to remain in the game — to be curious, to be present, to be needed, to be nourished.
And here’s the thought worth sitting with: every decade of life you’ve lived has been preparation for something. All of that accumulated experience, all those difficult years and surprising joys and hard-earned lessons — they didn’t expire at seventy-nine. They matured.
The question isn’t whether life after eighty is worth living fully. The question is whether you’ll let it be.
Discover more from MatterDigest
Subscribe to get the latest posts sent to your email.



